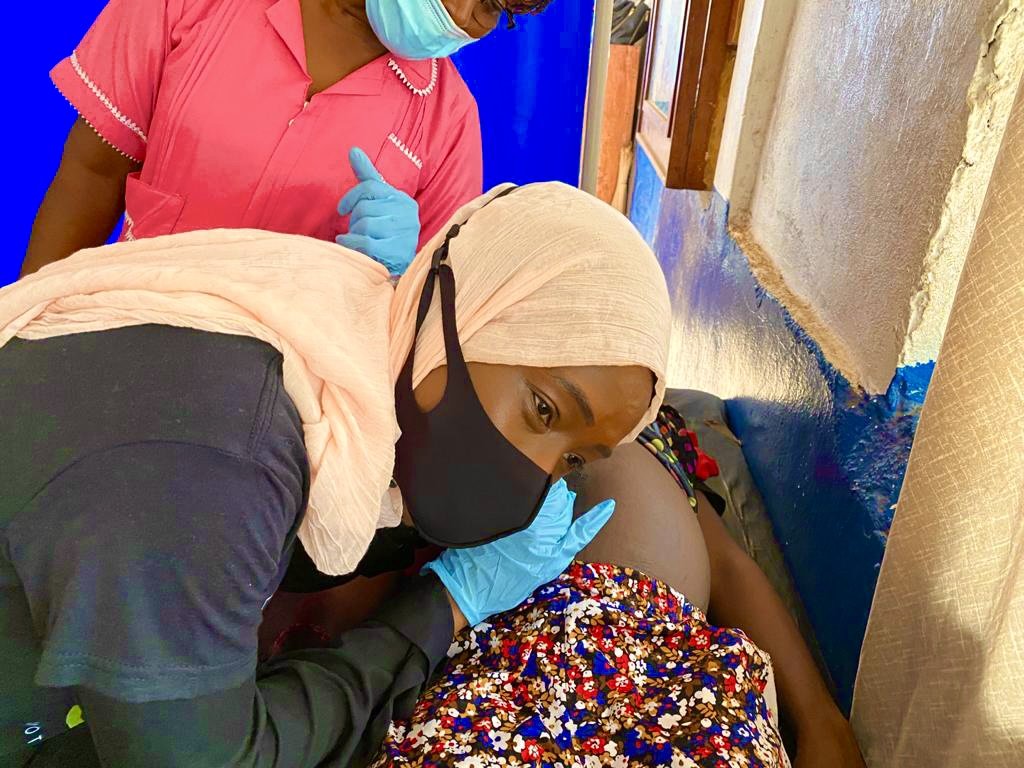
our work
One people, one fight #fightforourmothers
TMF AREA OF FOCUS
Transportation and Referral System (The "Second Delay"). While we have strong outreach and in-facility care, a common point of failure for rural maternal health is the inability to transport a woman with a complication to a higher-level facility (hospital) in time. Commonly known as the "Second Delay." Areas to Strengthen:
● Emergency Transport Network: Our current programs help women deliver in our clinics, but we must solidify a 24/7 emergency referral system (transportation) to move women with complications (e.g., severe bleeding, eclampsia, obstructed labor) from clinics to the regional hospital. ○ Action: Formalize a clear protocol with dedicated, pre-paid emergency transport (e.g., motorbike ambulance, vehicle service) and a dedicated fund for referrals until we can purchase our own.
Retention of Skilled Staff and Local Management. We train staff and provide supplies, but the Human Resources for Health (HRH) challenge in rural Sierra Leone is chronic: staff are often underpaid or not paid at all, lack staff housing, and many of them lack passion. This undermines program sustainability. Areas to Strengthen:
● Incentives and Retention: We need to move beyond general training to implement a robust, long-term staff retention package for key personnel (midwives, nurses) in our rural clinics. ○ Action: Provide non-financial incentives like staff quarters, performance bonuses tied to quality metrics, and opportunities for advanced training/mentorship.
● Supervisory and Mentorship Cadres: Ensure the quality of training translates into sustained clinical competency. ○ Action: Establish a dedicated, frequent, and structured mentorship and clinical supervision model for our clinic staff. This ensures the skills from the Point-of-Care Ultrasound and other training remain sharp.
● Local Management Transition: After five years on the ground, local ownership must be more formalized. ○ Action: Develop an exit or transition plan by training local community or District Health Management Team (DHMT) representatives in operational management, budgeting, and supply chain oversight to take over certain programmatic elements (e.g., clinic feeding program management) in the next five years.
Postnatal Care and Integrated Psychosocial Support. Our programs have a strong focus on ANC and delivery, but the period after delivery is a significant risk for both mother and infant. Furthermore, our current programs do not yet address the pervasive issue of Maternal Mental Health. Areas to Strengthen:
● Robust Postnatal Care (PNC) Linkage: Maternal deaths often occur in the immediate postpartum period, and infant complications can be missed. ○ Action: Strengthen the follow-up system for PNC visits, especially home visits by Community Health Workers, to monitor for complications (e.g., postpartum hemorrhage, infection) and ensure infant feeding/wellness. ● Psychosocial Integration (Future Initiative): Introduce our planned maternal mental health service as a pilot program. Addressing mental distress will enhance all other programs by improving adherence to ANC education, facility delivery, and feeding protocols. ○ Action: Pilot the Integrated Perinatal Mental Health Screening and a community-based support program (as previously discussed) to improve the mother's overall "quality of life" (Mission).
● Data Quality and Utilization: We have many excellent programs, but we must ensure we are consistently capturing and using data to prove their impact on the final Maternal Mortality Rate (MMR). ○ Action: Establish a robust Monitoring and Evaluation (M&E) system that goes beyond output (e.g., # of birthing buckets distributed) to outcome (e.g., reduction in Postpartum Hemorrhage rates or ANC attendance vs. delivery complication rates).
Our partnered clinics
Panlap
health centre
This clinic covers 14 communities of over 7,000 in population. The clinic lacks running water, a proper ceiling, suitable cribs, ultrasound / doppler machines, plastics sheets for the delivery beds, do not provide food for patients and no medical transport.
bINKOLO COMMUNITY HEALTH CENTRE
Covering 15 communities and 9,552 people.
The clinic lacks quality medical equipment, inadequate staffing, inadequate infrastructure that forces them to do antenatal and postnatal care in one confined space, no sheets for postnatal beds, no
mattresses for their cribs, do not provide food for patients and no medical transport.
KABOMBEH VILLAGE CLINIC
This clinic covers 6 communities, with over 4,000 people.The community has strong cultural norms where pregnant women prefer to deliver at home, there is a significant lack of medical supplies and equipment, very confined space for deliveries and no medical transport.
KATHENEH MCHP
Covering 4 communities and 1,755 people.
KMCHP has one delivery bed with minimal to no equipment and no electricity. This is the basic and lowest level of care in the healthcare system.
Staff from the Masongbo CHC and the Panlap CHC THANK THE TMF DONORS!
solar installations
The Mansaray Foundation’s multi-stakeholder approach to reducing maternal mortality, partnered with GIZ to install solar systems in 4 health centers. These partnerships are essential as we take on this challenging task of reducing maternal deaths in rural Sierra Leone. The midwives will no longer use flashlights to deliver babies at night. We extend our sincere gratitude to GIZ for being part of the solution to improving the quality of care in Sierra Leone.






